Pseudo-thrombocytopenia can have several causes, of which a part is preanalytical. The presence of giant platelets, platelet satellitism, or platelet clumping due to agglutination or aggregation can, for example, all result in that a portion of the platelets is excluded from the PLT count (1). Spuriously low PLT counts caused by pre-analytical factors do not pose any risk to the patient per se but may lead to inappropriate platelet transfusions or delays in surgical procedures (2).
Giant platelets
Giant platelet disorder, or macrothrombocytopenia, includes a heterogeneous group of rare disorders, featuring abnormal giant platelets and thrombocytopenia. Affected patients have an increased tendency to bleeding due to that the platelets cannot aggregate properly to form a solid hemostatic plug as response to an injury to the vessel wall (3).
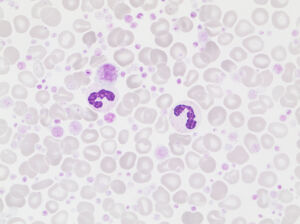
Pronounced PLT anisocytosis shown in the great numbers of platelets and some giant platelets , surrounding two neutrophil granulocytes.
As part of the complete blood count (CBC), Boule 3-part hematology analyzers report the concentration of platelets with a mean platelet volume larger than 12 fL.
The platelet large cell concentration (P-LCC) is defined as follows:
P-LCC = PLT × P-LCR
The large platelet concentration ratio (P-LCR) parameter is calculated from the PLT size distribution curve of diluted blood and is defined as follows:
P-LCR = Counted PLT particles larger than 12 fL / Total counted PLT particles
The effect of an excessive number of giant platelets, giving falsely low PLT and erroneously high RBC counts, is minimized by using a floating discriminator that estimates the best separation between cell populations. Boule 3-part hematology analyzers use a discriminator that floats between 10 and 28 fL, thereby preventing giant platelets to be falsely counted as RBCs.
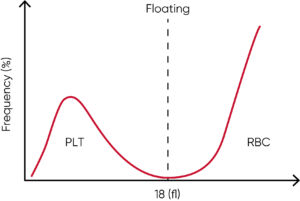
Floating discriminator technique prevents giant platelets to interfere with the RBC count.
Giant platelets interfering with the WBC differential count can be seen as a left shift of the LYM peak in Boule 3-part hematology analyzers, giving rise to a DE flag for small particle interference.
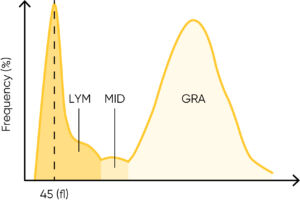
Boule 3-part hematology analyzers flag for a left shift in the LYM peak due to small particle interference (DE flag). A blood smear analysis can reveal the presence of NRBCs, PLT clumps, or giant platelets.
Platelet satellitism
Platelet satellitism is when platelets rosette around neutrophils, an in vitro phenomenon that can be observed under the microscope. The mechanism in not fully understood, but studies indicate that autoantibodies directed against the glycoprotein IIb/IIIa complex of the platelet membrane and the FcγRIIIA receptor of neutrophils are involved and that the bridge-formation is EDTA-dependent (5, 6).
The effect of platelet satellitism on the PLT count value is mitigated by the high dilution ratio (1:40 000) used for counting in Boule 3-part hematology analyzers.
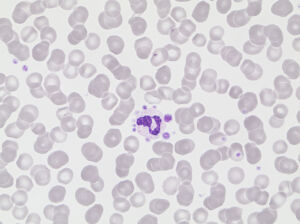
Platelet satellitism is an in vitro artifact found in anticoagulated blood in which platelets adhere to the periphery of neutrophils and sometimes even to monocytes. This phenomenon is difficult to detect from the histogram and is often detected as a chance finding by microscopy. New sample taken in sodium citrate is necessary for a correct platelet count.
Platelet clumping
Platelet clumping due to agglutination typically occurs at 4°C and is mediated by IgM autoantibodies directed against the glycoprotein complex IIb/IIIa on the platelet surface (1). As these antibodies have little or no activity at temperatures above 30°C, the phenomenon has no clinical significance. Instead, samples with suspected cold agglutination can be incubated for 15–30 min at room temperature to reverse the agglutination process before analysis.
Platelet clumping due to aggregation is often seen in patients with an ongoing blood clotting process and can, for example, be caused by the blood collection procedure. A low blood flow due to prolonged application of the tourniquet during venipuncture can cause hemoconcentration, increasing the opportunity for platelets aggregation (6, 7). It is recommended to mix the sample thoroughly to prevent platelet clumping before analysis.
When collecting capillary blood, it is important to achieve a good flow and to wipe away the first drop to minimize the risk of clotting and contamination of the sample with tissue fluid or debris (8).
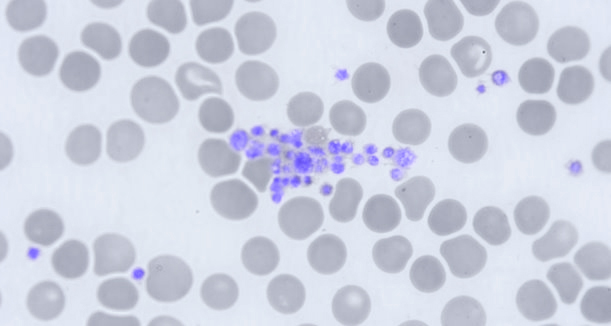
Platelet clumping due to aggregation.
In Boule 3-part analyzers, interference from clumping can be seen as an abnormal high at the lower discriminator of the RBC histogram.
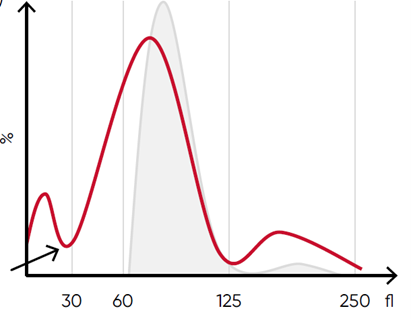
Possible causes of an RBC histogram showing an abnormal high at the lower discriminator can be RBC or WBC fragments, giant PLTs, microcytic RBC, or PLT clumps.
Conclusions
Analyzer flags and histograms are helpful indicators of the presence of platelet abnormalities that may cause spuriously low PLT counts. Yet, a low platelet count should be followed up by a blood spear analysis under the microscope.
References
- Wahed, A. and Dasgupta, A. in Hematology and Coagulation, Elsevier ISBN 978-0-12-800241-4 (2015).
- Bizzaro, N. in Platelets (3rd), Elsevier ISBN 978-0-12-387837-3 (2013).
- Andrea et al. Inherited platelet disorders: thrombocytopenias and thrombocytopathies. Blood Transfus 7, 278–292 (2009).
- Chakrabarti, I. Platelet satellitism: a rare, interesting, in vitro phenomenon. Indian J Hematol Blood Transfus 30, 213–214 (2014).
- Singh Bhar, V. and Singh, R. Platelet satellitism: unusual cause of spurious thrombocytopenia. J Hematop 12, 171–172 (2019).
- Blood collection guide by venipuncture for analytical purposes. OPTMQ, Québec, Canada ISBN: 978-2-9818452-1-4 (2020).
- Austin et al. Hemoconcentration and Hemostasis During Acute Stress: Interacting and Independent Effects. Ann Behav Med 42, 153–173 (2011).
- WHO Guidelines on Drawing Blood: Best Practices in Phlebotomy. World Health Organization, Geneva (2010).








